Author: Michael Vlessides
Anesthesiology News
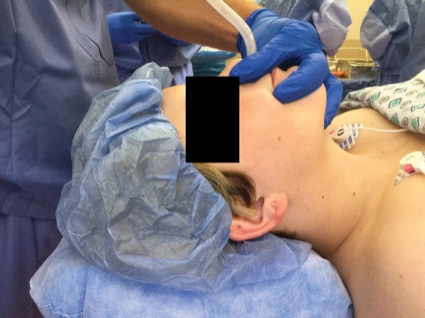
Nasopharyngeal ventilation, involving the placement of a regular endotracheal tube through the nose into the hypopharynx (Figure), is a viable alternative to mask ventilation in patients at risk for difficult mask ventilation, according to a new study. This technique, the researchers concluded, serves as a supraglottic airway, thereby offering an alternative ventilation method when intubating patients who have respiratory insufficiency.
While face mask ventilation is commonly used in patients with respiratory insufficiency until the airway can be secured with an endotracheal tube, the technique occasionally cannot be performed adequately, said Jerrad Businger, DO, an assistant professor of anesthesiology and critical care at the University of Louisville, in Kentucky. This increases the likelihood of inadequate oxygenation and increased airway-related morbidity and mortality, said Dr. Businger, the lead author of the study.
“With that in mind, we wanted to investigate the utility of nasopharyngeal ventilation as an alternative to mask ventilation, specifically in patients who were difficult to mask,” Dr. Businger said.
The researchers enrolled 40 surgical patients into the trial, consisting of 20 individuals who required direct nasal intubation (cohort A) and 20 others who met “difficult to mask ventilate” criteria (cohort B). “That was based on the requirement of three or more of the eight variables that we know that suggest difficulty with face mask ventilation,” Dr. Businger noted.
Patients in each group were randomly assigned to receive face mask ventilation followed by nasopharyngeal ventilation, or the reverse order, after anesthesia induction. Both a standard endotracheal tube and a standard face mask were used for each ventilation. “The key to successful nasopharyngeal ventilation is occluding both the oral airway and the nares, to ensure a nice seal when utilizing this method,” Dr. Businger said.
The researchers confirmed ventilation by the presence of end-tidal carbon dioxide waveforms, chest rise and fall, expired tidal volume, and peripheral oxygen saturation. Tidal volume was recorded for each breath for 60 seconds of ventilation.
Another Tool for the Armamentarium
“We found that in both cohort A and cohort B, there was a significant difference in terms of tidal volumes that we were able to deliver with the nasopharyngeal airway, compared with normal face mask ventilation,” Dr. Businger reported during the 2018 annual meeting of the International Anesthesia Research Society (abstract AM69). Indeed, tidal volume was significantly increased using the nasopharyngeal airway in both cohort A (597±156 vs. 456±230 mL; P=0.016) and cohort B (510±161 vs. 244±188 mL; P<0.01). With this approach, all patients were intubated successfully, and the researchers did not encounter significant desaturation or nasal bleeding in either cohort.
“This study goes to show that this nasopharyngeal airway should be in our airway management armamentarium in the operating room, especially in situations where you have difficulty with face mask ventilation,” he concluded.
Despite these promising results, some of Dr. Businger’s audience members questioned the applicability of the technique in various situations. “If you’re working alone, how difficult is it to make sure the mouth and nose are occluded while still doing everything else we need to do?” asked one attendee.
“It may be a little uncomfortable at first, in terms of getting used to the position required to accomplish all the tasks,” Dr. Businger replied. “But once you do it once, it becomes very easily accessible with one person.
“The key is getting a nice seal of the mouth and the nares,” he continued. “I still utilize this in practice and I’ve done it in many situations, even rescue situations.”
“One of the things we’ve done in some of our children is to use a nasal CPAP [continuous positive airway pressure] mask so you don’t have to insert a nasopharyngeal tube,” said Kumar Belani, MD, a professor of anesthesiology at the University of Minnesota Masonic Children’s Hospital, in Minneapolis. “The nasal CPAP/BiPAP [bilevel positive airway pressure] mask has worked well, especially if you anticipate a difficult upper airway.”
“We believe you can use the nasopharyngeal airway very easily during emergencies,” said study senior investigator Rainer Lenhardt, MD, MBA, a professor of anesthesiology at the University of Louisville, where he is the vice chair of clinical affairs. “A high-flow nasal cannula and CPAP are great tools, but you don’t have them readily available. “
“We use them for the anticipated difficult airway,” Dr. Belani replied. “For the unanticipated difficult airway, well, you’ve got to do what you’ve got to do.”


Leave a Reply
You must be logged in to post a comment.