Author: Bryan Sullivan
Chief Operating Officer, Plexus Technology Group, LLC, Fairfax, VA
F1rst News
As with previous years, the MIPS program is continuing to execute on its legislative mandate while also making accommodations for the COVID-19 pandemic. On July 13, 2021, CMS proposed changes for the 2022 reporting year; and, by the time you are reading this, it is possible this has been converted to the final rule. This review will highlight the important elements as they relate to the anesthesia and chronic pain specialties and will also focus on a few known items for future years.
The headline with the changes is that MIPS is likely to be decommissioned in five years. Before you get your hopes up, it is going to be replaced with a new hybrid approach called the MIPS Value Pathway or MVP. An MVP is essentially a new combined approach for reporting quality and performance metrics to CMS where categories of MIPS are combined into a single “track.” The program will have several options for anesthesia and chronic pain in the years to come, but you can think about it today as a lesser burden on reporting where you will not have to report six quality metrics and several improvement activities amounting to six to ten measures.
Overall, the future iteration of MIPS reflects an approach designed to reduce the provider’s burden and combine the entire program into six measures where some are quality-centric, some are improvement activity-centric and some are performance-centric. If you are interested in learning more about this, you can visit the CMS website, which explains a few details. Currently, however, there is only one MVP approved for 2022, so there is not a lot of variety just yet
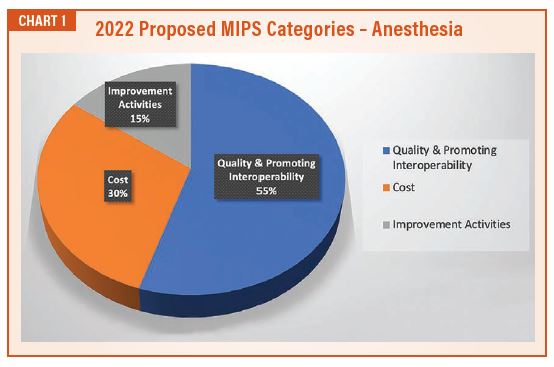
As for additional specifics of the MIPS program for 2022, the Quality and the Cost categories are now reweighted to 30 percent each, while the Promoting Interoperability and Improvement Activity categories remain the same at 25 percent and 15 percent, respectively. For anesthesia, however, the promoting interoperability category is exempted, and those points will be combined with the Quality category yielding an adjusted weight of 55 percent.
The other major difference for 2022 is that the performance threshold is now fluid. This means that there is no longer a floor percentage that practices and providers must achieve for penalty avoidance. Rather, CMS will take the mean or median score which they expect to be at 75 MIPS points. This is a substantial increase over 2021, which had a floor of 60 MIPS points, and it will be absolutely critical for those providers reporting to ensure they achieve this level. We also remind all providers to validate your reporting requirement, as well, as it may no longer be beneficial to continue reporting if you are no longer required to. Finally, the penalty will remain consistent with 2021 at +/- nine percent of MIPS allowed charges.
 Regarding the Quality measures, only one anesthesia measure is being considered for removal, which is MIPS 44 – Coronary Artery Bypass Graft (CABG): Preoperative Beta-Blocker in Patients with Isolated CABG Surgery. No other changes to the anesthesia measures are currently proposed, but there are several being considered that may affect chronic pain. We will send out notifications regarding any changes on these that may become final.
Regarding the Quality measures, only one anesthesia measure is being considered for removal, which is MIPS 44 – Coronary Artery Bypass Graft (CABG): Preoperative Beta-Blocker in Patients with Isolated CABG Surgery. No other changes to the anesthesia measures are currently proposed, but there are several being considered that may affect chronic pain. We will send out notifications regarding any changes on these that may become final.
The other major consideration is hardship exemptions for those providers who are affected by the COVID-19 pandemic. Currently, an automatic exemption is not available for 2021, and nothing has been released for 2022 as of this writing. Providers are encouraged to continue reporting as required by rule to avoid any penalties, should one become relevant. As always, we are here as your partner in this Quality Payment Program journey and want to ensure that our clients, our practices and our specialty succeed with the government programs of today and of tomorrow!


Leave a Reply
You must be logged in to post a comment.