Author: Tony Mira
F1rstNews
Summary: The anesthesia specialty is critical to America’s overall healthcare system. However, according to a newly released study, the nation is facing a growing dearth of anesthesia providers.
The hot topic of the day is the shortage in anesthesia manpower. Not since the 1990s with the publication of the Abt Corporation report has there been such concern about the dwindling supply of anesthesia providers. Some of us remember the publication of that report and its claim that there would be a surplus of anesthesia providers in the coming years. This belief led many second- and third-year residents at that time to opt for other specialties. It took the anesthesia specialty quite a number of years to recover. Now we are experiencing another shortage, and many people are asking if it’s real and, if so, why is it happening.
Some Facts
A recent study from the RAND corporation predicted that the gap in anesthesiology services will be just as important to Americans’ health as the projected gap for primary physician services. In other words, the shortage will ultimately impact the ability to schedule surgical cases, and patients will have to start waiting longer periods for elective surgeries. RAND is a professional organization, and this broad-based study took all significant aspects of anesthesia care into consideration.
According to RAND, there are approximately 35,000 practicing anesthesiologists and an equal number of CRNAs. The RAND conclusion is that there is currently a shortage of about 3,800 anesthesiologists and 1,280 CRNAs, representing a 9.8 percent shortage of physicians and a 3.8 percent shortage of nurse anesthetists. The projection is that, if current trends continue, this will increase to a shortage of 4,500 physicians and 8,000 CRNAs within the next ten years. The chart below illustrates the RAND findings by region of the country.
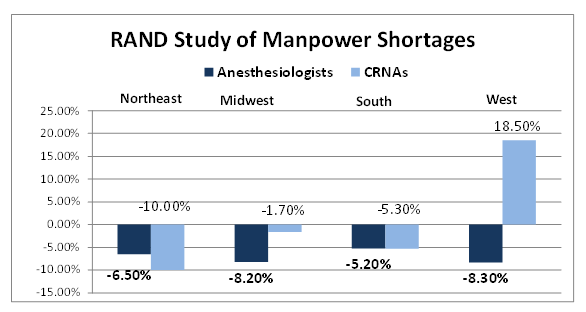
Some Answers
There are no crystal-clear answers as to why there is a shortage of anesthesia providers, but there are a number of key factors that definitely contribute to the current state of affairs. The first of these is clearly the migration of so many cases from traditional inpatient venues to outpatient and ambulatory venues. This trend has increased the number of anesthesia providers. Not only has this increased the number of anesthetizing locations that have to be covered, but it has reduced the overall average productivity of locations. Not only that, it has increased the disparity between hospital venues (which tend to have a much higher Medicare and Medicaid population) and ASCs (which tend to have a much more favorable payer mix of commercial cases). The result is that the coverage requirements of hospitals end up necessitating ever larger subsidies.
Many facilities are also seeing an increase in NORA activity. Anesthesia providers are being called on to cover a wider range of non-OR sites, where the scheduling is much less predictable and sporadic. It is not uncommon for groups to have to schedule an additional provider just to cover NORA activity.
There is no question that today’s providers are more mobile than ever in the past. The younger generation, in particular, is more willing to simply pick up and move if a situation does not meet their income and lifestyle expectations. To some extent, this may have been encouraged by the large national staffing companies because they allow providers the flexibility of being able to move from one service location to another.
Many clients also cite provider burnout as a key factor, especially in light of the Covid-19 experience last year. Clearly, we are seeing more anesthesia providers retire early. They are just not willing to deal with current workloads and compensation.
What the Future Holds
The RAND study is not encouraging. It appears that anesthesia has lost its luster as a preferred clinical specialty. The problem is that such trends tend to spiral downward. Levels of frustration and dissatisfaction tend to discourage new providers from choosing the specialty. Only time will tell if the specialty turns this around.


Leave a Reply
You must be logged in to post a comment.