Source: Cardiac Anesthesiologist blog
An Updated Report by the American Society of Anesthesiologists Task Force on Prevention of Perioperative Peripheral Neuropathies
I. Preoperative History and Physical Assessment
• When judged appropriate, it is helpful to ascertain that patients can comfortably tolerate the anticipated operative position.
• Body habitus, preexisting neurologic symptoms,
diabetes mellitus, peripheral vascular disease, alcohol dependency, arthritis, and gender (e.g., male gender and its association with ulnar neuropathy) are important elements of a preoperative history.
II. Positioning Strategies for the Upper Extremities
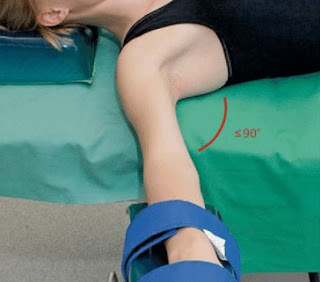
• Arm abduction in supine patients should be limited to 90 degrees. Patients who are positioned prone may comfortably tolerate arm abduction greater than 90 degrees.
• Supine Patient With Arm on an Arm Board: The upper extremity should be positioned to decrease pressure on the postcondylar groove of the humerus (ulnar groove). Either supination or the neutral forearm positions facilitates this action.
 • Supine Patient With Arms Tucked at Side: The forearm should be in a neutral position. Flexion of the elbow may increase the risk of ulnar neuropathy, but there is no consensus on an acceptable degree of flexion during the perioperative period. Prolonged pressure on the radial nerve in the spiral groove of the humerus should be avoided. Extension of the elbow beyond the range that is comfortable during the preoperative assessment may stretch the median nerve. Periodic perioperative assessments may ensure maintenance of the desired position.
• Supine Patient With Arms Tucked at Side: The forearm should be in a neutral position. Flexion of the elbow may increase the risk of ulnar neuropathy, but there is no consensus on an acceptable degree of flexion during the perioperative period. Prolonged pressure on the radial nerve in the spiral groove of the humerus should be avoided. Extension of the elbow beyond the range that is comfortable during the preoperative assessment may stretch the median nerve. Periodic perioperative assessments may ensure maintenance of the desired position.
III. Specific Positioning Strategies for the Lower Extremities
• Stretching of the Hamstring Muscle Group: Positions that stretch the hamstring muscle group beyond the range that is comfortable during the preoperative assessment may stretch the sciatic nerve.
• Limiting Hip Flexion: Because the sciatic nerve or its branches cross both the hip and the knee joints, extension and flexion of these joints, respectively, should be considered when determining the degree of hip flexion. Neither extension nor flexion of the hip increases the risk of femoral neuropathy. Prolonged pressure on the peroneal nerve at the fibular head should be avoided.
IV. Protective Padding
• Padded Arm Boards: Padded arm boards may decrease the risk of upper extremity neuropathy
• Chest Rolls: The use of chest rolls in the laterally positioned patient may decrease the risk of upper extremity neuropathy.
• Padding at the Elbow: Padding at the elbow may decrease the risk of upper extremity neuropathy.
• Padding to Protect the Peroneal (Fibular) Nerve: The use of specific padding to prevent pressure of a hard surface against the peroneal nerve at the fibular head may decrease the risk of peroneal neuropathy.
• Complications From the Use of Padding: The inappropriate use of padding (e.g., padding too tight) may increase the risk of perioperative neuropathy.
V. Equipment
The use of properly functioning automated blood pressure cuffs on the arm (i.e., placed above the antecubital fossa) does not change the risk of upper extremity neuropathy. The use of shoulder braces in a steep head-down position may increase the risk of perioperative neuropathies.
VI. Postoperative Assessment
A simple postoperative assessment of extremity nerve function may lead to early recognition of peripheral neuropathies.
VII. Documentation
Documentation of specific perioperative positioning actions may be useful for continuous improvement processes and may result in improvements by helping practitioners focus attention on relevant aspects of patient positioning and providing information on positioning strategies that eventually leads to improvements in patient care.


Leave a Reply
You must be logged in to post a comment.