Author: Michael Vlessides
Anesthesiology News
Ambulatory knee arthroscopy can be performed successfully under regional anesthesia in minimally sedated, awake patients with or without the use of a supplemental audiovisual device, according to a pilot study by a team of New York researchers. Patients in both groups received midazolam, although fewer patients with audiovisual distraction asked for supplemental sedation.
“Regional anesthetic techniques can provide sufficient surgical anesthesia,” said Lukas Pichler, MD, a research fellow at the Hospital for Special Surgery and NewYork-Presbyterian/Weill Cornell Medicine, in New York City. “However, patients often require sedation because of anxiety related to seeing or hearing things. Nevertheless, the use of sedatives is associated with a variety of side effects, which can include delirium, hemodynamic derangement, airway obstruction, aspiration and in extreme cases, airway loss.
“Therefore, reducing or eliminating sedatives may lead to improved perioperative outcomes,” Dr. Pichler continued. “So, distracting the patient with music or with audiovisual devices may reduce anxiety and also sedative requirements.”
To help determine the feasibility of using audiovisual devices, in this case video goggles, in this patient population, Dr. Pichler and his colleagues enrolled 26 individuals into the trial, all of whom were undergoing primary, ambulatory arthroscopic meniscectomy under spinal anesthesia. Patients were randomly assigned to receive minimal sedation with (n=13) or without (n=13) the use of audiovisual devices.
All patients received 2 mg of midazolam before placement of the spinal anesthetic, and were allowed to request additional sedation at any time. Pain scores and State-Trait Anxiety Inventory scores were recorded at baseline and after surgery. The Heidelberg Peri-anesthetic Questionnaire and the Client Satisfaction Questionnaire were used to gauge patient satisfaction. A questionnaire was also created for anesthesiologists and surgeons to provide feedback on their experience using the video goggles.
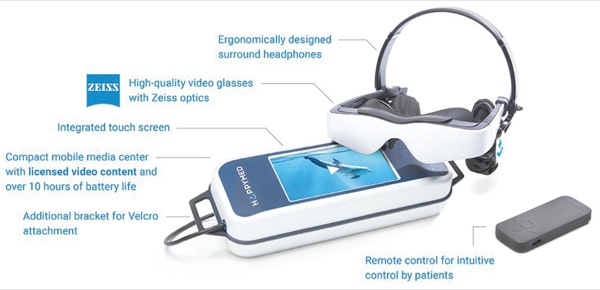
“Patients in the intervention group wore audiovisual devices and chose videos before being transported to the OR [operating room],” Dr. Pichler said in presenting the study at the 2018 Joint World Congress on Regional Anesthesia and Pain Medicine and annual meeting of the American Society of Regional Anesthesia and Pain Medicine (abstract 5717). “The device was essentially a set of video goggles and headphones that are connected to either a tablet or special device that was custom made for this purpose” (Figure).
The study found no differences between groups in postoperative pain scores or consumption of opioids and other analgesics (Table). Five patients in the control group and three in the audiovisual group requested additional sedatives during the case; this difference was not significant. Two additional patients in the audiovisual group received additional sedatives, per the anesthesiologist’s assessment.
| Table. Patient Outcomes With and Without Use of an Audiovisual Device | ||||
| AVD, 13 Patients | No AVD, 13 Patients | Difference in Means or Odds Ratio (95% CI) | P Value | |
|---|---|---|---|---|
| Patient request for additional sedatives, n (%) | 3 (23.1) | 5 (38.5) | 0.60 (0.18-2.01) | 0.673 |
| Administration of additional sedatives, n (%) | 5 (38.5) | 5 (38.5) | 1.00 (0.38-2.64) | 0.999 |
| Maximum intraoperative change from baseline SBP (mm Hg), mean ± SD | 7±14 | 7±10 | 0 (–10 to 10) | 0.987 |
| Maximum intraoperative change from baseline DBP (mm Hg), mean ± SD | 2±7 | 3±8 | –1 (–7 to 5) | 0.727 |
| Maximum intraoperative change from baseline HR (beats/minute), mean ± SD | 17±11 | 17±27 | 0 (–17 to 17) | 0.970 |
| Opioid use (mg OME), mean ± SD | ||||
| Intraoperative | 3.5±12.5 | 2.3±8.3 | 1.2 (–6.7 to 9.0) | 0.773 |
| Inpatient postoperative | 10.8±5 | 9.8±6 | 1.0 (–3.1 to 5.1) | 0.645 |
| AVD, audiovisual device; DBP, diastolic blood pressure; HR, heart rate; OME, oral morphine equivalents; SBP, systolic blood pressure | ||||
“We demonstrated that performing ambulatory knee surgery under regional anesthesia in awake patients is feasible both with and without the use of audiovisual devices,” Dr. Pichler said. “Then again, this was a pilot study, and it was not designed to demonstrate the superiority of audiovisual distraction. Therefore, future studies should use greater sample sizes to determine if audiovisual distraction can reduce the requirement for sedatives and improve postoperative outcomes.”
Increasing Research Volume
In fact, the investigators are enrolling patients for a larger trial. “That study will investigate the use of audiovisual devices in patients with obstructive sleep apnea undergoing knee arthroplasty surgery, because they are at higher risk of adverse events from sedatives,” Dr. Pichler pointed out.
“The patients did get to choose from a variety of content,” Dr. Pichler replied.
Despite these positive results, session moderator Alexandru Visan, MB, MBA, noted that similar results could be obtained by using propofol sedation with regional anesthesia. “Some practices that want to get the most out of a regional anesthetic without much sedation simply use propofol,” said Mr. Visan, the CEO of Executive Cortex Consulting, in Miami. “The patient wakes up at the end of the case and then five or 10 minutes later, they’re out of the OR, with or without audiovisual interactions.”
“I have also used propofol for sedation in many cases because of its short half-life,” Dr. Pichler replied. “However, those patients were not awake. We specifically wanted to conduct awake surgery.”
“There’s a strong argument that regional anesthesia should not be used for awake surgery because it’s not an anesthetic in its entirety,” Dr. Visan continued. “It’s an argument that I think will continue for a long time, but I don’t think it’s a bad thing if patients are asleep for the entire case.”


Leave a Reply
You must be logged in to post a comment.