Anesthesiology News
Director, Obstetric Anesthesia
Department of Anesthesiology
Penn State College of Medicine
Penn State Milton S. Hershey Medical Center
Hershey, Pennsylvania
Difficult and failed tracheal intubation in obstetric patients is a well-known problem with potentially devastating consequences. Fortunately, the recently reported incidence of fatalities related to failed intubation in the parturient is declining.1-7 This has been attributed to improved preoperative airway assessment and preparedness, better clinical and simulation training, and the availability of advanced airway technology such as video laryngoscopy and supraglottic airway devices (SADs).
In addition, the widespread use of guidelines and algorithms has significantly contributed to a safer environment for the airway management of the parturient. In a landmark study published in 1997 in which Hawkins et al analyzed data from 1979 to 1990, airway-related problems were reported to have led to maternal fatalities in 52% of cases.8 The same author then published a follow-up study in 2011 in which data from 1991 to 2002 were analyzed, which showed that anesthesia-related mortality had decreased by 60%. Mortality rates were similar for general and regional anesthesia.9
“The difficulty encountered during laryngoscopy and the inability of an experienced anesthesia practitioner to intubate within the time provided by one dose of succinylcholine.”
… and failed intubation as:
“The inability to secure the airway with two attempts, which includes the best attempt at intubation using the conventional laryngoscope or the use of an alternative airway device to assist with tracheal intubation.”10
The Table summarizes the definitions used for failed intubation in selected articles.
| Table. Selected Articles Defining Failed Intubation in Obstetric Patients | ||
| Definition of Failed Intubation | Incidence | Author |
|---|---|---|
| “Failure to achieve tracheal intubation during a rapid sequence induction for obstetric anaesthesia, thereby initiating a failed intubation drill.” | 1:224 | Quinn et al2 |
| ‘‘Inability to secure the airway after a single dose of succinylcholine and no more than two attempts at intubation using a conventional laryngoscope or an alternative airway device.” | 1:232 | Rajagopalan et al3 |
| “Intubation that was not accomplished with a single dose of succinylcholine.” | 1:249 | Barnardo et al4 |
| “Unsuccessful attempts at placement of an endotracheal tube into the trachea using either direct laryngoscopy or alternative intubating equipment, the need to proceed with surgery with a non-elective unsecured airway … or the need to abort intubation or surgery and awaken the woman prior to surgery.” | 1:154 | McKeen et al5 |
| “The inability to intubate the trachea and the subsequent abandonment of intubation as a means of airway management.” | 0 | Djabatey et al6 |
The Society for Obstetric Anesthesia and Perinatology Research Committee coordinated a review of 257,000 anesthetics performed in 30 institutions between October 2004 and June 2009 (SCORE study).7 Five thousand cases of general anesthesia for cesarean delivery (CD) were identified. Within that cohort, there was an incidence of failed intubation of 1:553 cases. In patients with a failed intubation, there were no hypoxemic arrests.7
McKeen et al define failed intubation in obstetric patients as the “inability to secure the airway after a single dose of succinylcholine and no more than two attempts at intubation using a conventional laryngoscope or an alternative airway device.”5 Rajagopalan et al retrospectively reviewed airway management for CDs performed between 2006 and 2013. The authors, using this definition, reported a 1:232 incidence of failed intubation. In all cases of failed intubation in this series, the airway was successfully managed with use of a laryngeal mask airway.3
General anesthesia is the fastest approach to reliably anesthetize a patient for a category 1 CD, meaning there is an immediate threat to the life of the mother or baby.11 The longer time associated with establishing neuraxial anesthesia in cases of emergent CD for fetal compromise can result in both delay in delivery and neonatal morbidity.12 In a recent systematic review of meta-analyses, Krom et al demonstrated that, in patients with an anticipated difficult airway undergoing category 1 CD for fetal distress, surgical anesthesia was established with general anesthesia using rapid sequence induction and video laryngoscopy in a significantly shorter time (100 seconds) than spinal anesthesia (6.3 minutes).11
Reluctance to convert an inadequate neuraxial anesthetic to general anesthesia frequently results in maternal pain or discomfort and emotional distress. This leads to decreased patient satisfaction and increased liability for the anesthesiologist.1,12 Szypula et al analyzed litigation related to regional anesthesia in the United Kingdom and found that pain during CD or labor was the most common “damaging event” in obstetric patients (57/186 claims).13
With the declining rate of general anesthesia for CD, familiarity with the obstetric airway is decreasing. The choice of anesthetic for CD, as reported between 2010 and 2015 in the National Anesthesia Clinical Outcomes Registry (NACOR), demonstrated that only 5.8% of CDs in the United States are performed under general anesthesia.14
The implication of this statistic is that there are anesthesia residents graduating without hands-on experience providing general anesthesia for CD.14,15 Simulation-based teaching has been criticized for a lack of reproducibility of the stressful environment associated with the extreme urgency of a CD. However, as shown by Balki et al, didactic teaching combined with repeated high-fidelity simulation sessions with a validated checklist improved the technical and nontechnical skills of anesthesia residents in that setting.16
Role of Video Laryngoscopy In Managing the Obstetric Airway
Video laryngoscopy offers the advantage of improved glottic visualization and a higher first-attempt endotracheal intubation success rate in both predicted and unexpected difficult airways. Its use also is associated with a high success rate of rescue intubation. The American Society of Anesthesiologists (ASA) “Practice Guidelines for Management of the Difficult Airway” recommend considering video-assisted laryngoscopy as an option for the initial approach to intubation in the general population, on the basis of the anesthesiologist’s skill and preference.17It is not clear whether this should be applied to all cases of general anesthesia in the obstetric patient. In a review article on management of the unexpected difficult intubation in pregnant patients, Mhyre and Healy recommended using video laryngoscopes as backup devices after a failed attempt to intubate the trachea with direct laryngoscopy.18
There are many reports of the successful use of video laryngoscopes for initial intubation in obstetric patients with a normal or predicted difficult airway, or as rescue devices after failed direct laryngoscopy.19-23 However, comparative studies in the obstetric population are lacking.
A retrospective analysis by Aziz et al reported the successful use of the GlideScope (Verathon) to intubate the trachea in all patients on the first attempt.20 Shonfeld et al described the successful use of the C-MAC (KARL STORZ Endoscopy) in 27 patients.21 The Airway Scope (Pentax) has been described as a successful rescue device after failed intubation, and was used to intubate 2 patients for unscheduled intraoperative awake endotracheal intubation during CD.22,23
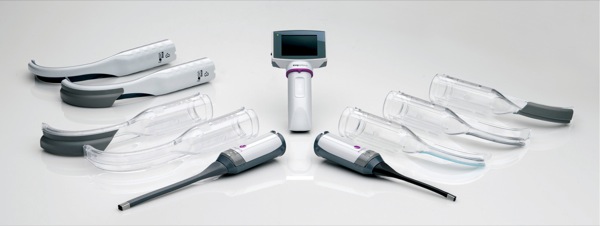
Technological advances have been made in the design of several video laryngoscopes to include obstetric airway–friendly features to address the special need for short-handled laryngoscopes. The laryngoscope blade of the King Vision (Ambu) portable video laryngoscope (Figure) can be inserted separately, and, once positioned in the oropharynx, the monitor can be attached. That can be an advantage when intubating an obstetric patient, as breast engorgement may interfere with placement of the laryngoscope.
Pharyngeal trauma has been associated with the use of video laryngoscopes, requiring a stylet to facilitate intubation.24 The increased upper airway tissue friability seen in obstetric patients might make them more prone to this complication. A potential disadvantage of video laryngoscopy is the longer time required to intubate the trachea compared with conventional laryngoscopy.25,26 The prolonged period of apnea may be problematic in obstetric patients who desaturate quickly due to increased oxygen consumption and decreased functional residual capacity. To date, there is no evidence that this longer period of apnea is of any clinical significance.
Role of Supraglottic Airway Devices In Managing the Obstetric Airway
In a difficult intubation situation, adequate oxygenation and ventilation take priority over endotracheal intubation. Failed intubation must be declared after 2 unsuccessful attempts to intubate the trachea with direct or video laryngoscopy.
SADs (both laryngeal mask and non-laryngeal mask airways) have been evolving continually. These improvements have resulted in safer tools for airway management. SADs should be used early in the airway algorithm to minimize the risk for airway trauma and hypoxia. No more than 2 attempts at supraglottic ventilation are allowed. Cricoid pressure should be released transiently to facilitate successful placement of a SAD. Optimal SAD size selection, depth of insertion, and cuff inflation are crucial for the proper functioning of SADs. Insufficient cuff inflation causes hypoventilation, whereas overinflation can cause damage to surrounding tissues.
SADs are typically inserted blindly, often resulting in the malposition of the device.27
However, even suboptimally positioned SADs can still provide airway patency, oxygenation, and ventilation for short procedures. Suboptimal positioning of a SAD can be corrected by adjusting the head/neck position, applying jaw lift, or changing the depth of insertion. Clinically, airway patency is verified by bilateral chest auscultation, capnography, pulse oximetry, airway pressure, and oropharyngeal sealing pressure. Additionally, the ability to ventilate patients with airway pressure greater than 20 cm H2O correlates with a correct SAD position. Preference should be given to second-generation SADs that separate the alimentary and respiratory tracts (eg, Laryngeal Mask Airway [LMA] Supreme [Teleflex]), as they provide greater airway protection over first-generation SADs.
The LMA (Teleflex) and its variants are by far the most frequently used SADs; however, other SADs should be available for those situations where they have failed to oxygenate and ventilate. Ramachandran et al reported an incidence of 1.1% failure after the elective use of the LMA Unique (Teleflex) in a general population. These patients presented a 3-fold increased incidence for difficult mask ventilation.28
Alternative SADs with different designs and performance characteristics may provide adequate oxygenation and ventilation in circumstances where a laryngeal mask airway fails. For this reason, anesthesiologists should be familiar with at least one additional SAD other than a laryngeal mask airway and prepared to use it in cases of an unexpected difficult airway where the laryngeal mask airway or mask ventilation fails. Among numerous available SADs, the choice should be made on the basis of availability, user preference, and expertise. Achieving proficiency and retaining the skills necessary to efficiently use an alternative noninvasive airway device may prove to be crucial in a life-threatening “cannot intubate, cannot oxygenate” scenario.
The choice among the numerous available SADs should be determined by availability, proficiency, and user preference. Again, preference should be given to second-generation SADs with an esophageal drain. They can be supraglottic (eg, LMA Supreme, i-gel [Intersurgical]) or retroglottic airways with 2 inflatable cuffs (eg, King LT-D [Ambu]). The LMA Protector (Teleflex) is a new second-generation SAD designed to minimize the risk for aspiration by channeling gastric contents away from the airway. It has a pharyngeal chamber, dual gastric channels to remove fluids from the airway, and an integrated cuff pressure indicator. To date, there have been no reports of the use of the LMA Protector in obstetric patients.
If adequate oxygenation and ventilation are possible, a SAD may be left in situ until the completion of the CD. A SAD may be left in place for several hours, but the length of time of safe ventilation is still being investigated. The decision to leave a SAD in place or proceed to an exchange with an endotracheal tube after delivery should be based on the adequacy of oxygenation and ventilation, the expected length of surgery, and the anesthesiologist’s familiarity with the SAD. The surgeon should be advised to apply gentle fundal pressure during the delivery of the newborn.18 Exchanging a SAD for an endotracheal tube can be challenging, but losing the airway has life-threatening consequences. Several techniques to facilitate tracheal intubation through a SAD have been described, including blind intubation or facilitation by light wands, optical stylets, or a fiber-optic bronchoscope.29
Role of Ultrasonography in Managing the Obstetric Airway
Ultrasonography of the upper airway is steadily becoming a simple, bedside-accessible noninvasive tool to help evaluate the airway. Recently, Ahuja et al described the use of airway sonography to assess dynamic airway dimensional changes in pregnant patients. The authors reported an “increase in soft tissue thickness at the level of the hyoid bone after labor” in both normotensive and preeclamptic patients.30
Identifying the cricothyroid membrane (CTM) is challenging, especially in an emergency. Ultrasonography can be used to reliably guide the preemptive location of the CTM to facilitate front-of-neck access, should it be necessary.19 Gadd et al reliably used airway ultrasonography to measure the CTM depth in normal-weight and obese pregnant patients, showing a close linear relationship between the CTM depth and neck circumference.31
Managing Extubation in the Parturient
Airway changes during pregnancy and labor are progressive and persist into the postpartum period. For that reason, the same planning and precautions taken for airway management in the prepartum patient should be followed for extubation and for at least 48 hours after delivery.
Myhre et al reviewed anesthesia-related maternal deaths in Michigan between 1985 and 2003. Eight fatalities were anesthesia related, with all cases of death due to airway problems (airway obstruction or hypoventilation) occurring during emergence and recovery from anesthesia. No airway-related deaths occurred during the induction of anesthesia.32
The ASA “Practice Guidelines for the Management of the Difficult Airway” emphasize the importance of a “pre-formulated extubation strategy.”17 In 2012, the Difficult Airway Society (DAS) in the United Kingdom published guidelines for the management of tracheal extubation, which highlighted the importance of a stepwise approach that includes planning, preparing, and executing tracheal extubation, and should include post-extubation follow-up.33 The successful use of an airway exchange catheter (AEC) for staged extubation has been described in a pregnant patient with an unexpected difficult intubation.34 AECs are well tolerated by awake and spontaneously breathing patients, and should be considered to increase extubation safety in pregnant patients with difficult intubation and/or suspected difficult extubation.
Obstetric-Specific Algorithms for Managing Difficult and Failed Intubation
Recently developed guidelines and algorithms offer a systematic approach and practical advice for managing the difficult airway in obstetric anesthesia. The Obstetric Anaesthetists’ Association and DAS have published guidelines that include steps to “optimize a safe general anesthetic technique in the obstetric patient” and discuss management “after declaring failed tracheal intubation” as well as in the “‘cannot intubate, cannot oxygenate’ situation, and emergency front-of-neck airway access.”
The question of whether to awaken the mother after failed intubation or proceed with general anesthesia with the airway efficiently secured with a SAD or adequate face mask ventilation is addressed separately.18 Strong indications for awakening the mother are hypoxemia, an obstructed airway, and inadequate capnography. Successful implementation of algorithms requires frequent simulation-based training with institutionally available airway equipment.
The Vortex concept has been developed by Chrimes as a visual cognitive aid to help implement difficult airway management algorithms.35 The Vortex graphical representation of looking down into a funnel symbolizes the rapid and progressive deterioration of an airway crisis toward the “blue zone,” representing the life-threatening situation of a cannot intubate, cannot oxygenate scenario. The “green zone” of the Vortex is reached by reestablishing airway patency, offering the opportunity to reorganize and make a plan.35 However, there are no reports of implementing the Vortex approach in obstetric anesthesia.
Conclusion
The incidence of failed intubation in obstetric anesthesia is significantly higher than in the general population. Recently developed guidelines and algorithms offer a systematic approach for managing the difficult airway in obstetric anesthesia. With further technological advances and operator comfort, video laryngoscopes will likely become the first option for the initial approach to intubation for CD. With an emphasis on adequate oxygenation rather than endotracheal intubation, SADs should be used early in the airway algorithm. When considering a SAD, preference should be given to those that are second-generation SADs.
There are serious and ethical concerns with studying obstetric difficult airway management in prospective randomized controlled trials. Thus, the decision of whether video laryngoscopes should be used as a primary airway device for initial intubation in obstetric patients undergoing general anesthesia is not likely to be based on evidence anytime soon.
Acknowledgment: The author thanks Daniel Vaida for helping with the editing process.
References
- Hawkins JL. Excess in moderation: general anesthesia for cesarean delivery. Anesth Analg. 2015;120(6):1175-1177.
- Quinn AC, Milne D, Columb M, et al. Failed tracheal intubation in obstetric anaesthesia: 2 yr national case-control study in the UK. Br J Anaesth. 2013;110(1):74-80.
- Rajagopalan S, Suresh M, Clark SL, et al. Airway management for cesarean delivery performed under general anesthesia. Int J Obstet Anesth. 2017;29:64-69.
- Barnardo PD, Jenkins JG. Failed tracheal intubation in obstetrics: a 6-year review in a UK region. Anaesthesia. 2000;55(7):690-694.
- McKeen DM, George RB, O’Connell CM, et al. Difficult and failed intubation: incident rates and maternal, obstetrical and anesthetic predictors. Can J Anaesth. 2011;58(6):514-524.
- Djabatey EA, Barclay PM. Difficult and failed intubation in 3430 obstetric general anaesthetics. Anaesthesia. 2009;64(11):1168-1171.
- D’Angelo R, Smiley RM, Riley ET, et al. Serious complications related to obstetric anesthesia: the serious complication repository project of the Society for Obstetric Anesthesia and Perinatology. Anesthesiology. 2014;120(6):1505-1512.
- Hawkins JL, Koonin LM, Palmer SK, et al. Anesthesia-related deaths during obstetric delivery in the United States, 1979-1990. Anesthesiology. 1997;86(2):277-284.
- Hawkins JL, Chang J, Palmer SK, et al. Anesthesia-related maternal mortality in the United States: 1979-2002. Obstet Gynecol. 2011;117(1):69-74.
- Suresh MS, Wali A, Munnur U. Airway management in obstetric patients. In: Hagberg CA, Artime CA, Aziz MF, eds. Hagberg and Benumof’s Airway Management. 4th ed. New York, NY: Elsevier; 2018:641.
- Krom AJ, Cohen Y, Miller JP, et al. Choice of anaesthesia for category-1 caesarean section in women with anticipated difficult tracheal intubation: the use of decision analysis. Anaesthesia. 2017;72(2):156-171.
- Davies JM, Posner KL, Lee LA, et al. Liability associated with obstetric anesthesia: a closed claims analysis. Anesthesiology. 2009;110(1):131-139.
- Szypula K, Ashpole KJ, Bogod D, et al. Litigation related to regional anaesthesia: an analysis of claims against the NHS in England 1995-2007. Anaesthesia. 2010;65(5):443-452.
- Juang J, Gabriel RA, Dutton RP, et al. Choice of anesthesia for cesarean delivery: an analysis of the National Anesthesia Clinical Outcomes Registry. Anesth Analg. 2017;124(6):1914-1917.
- Palanisamy A, Mitani AA, Tsen LC. General anesthesia for cesarean delivery at a tertiary care hospital from 2000 to 2005: a retrospective analysis and 10-year update. Int J Obstet Anesth. 2011;20(1):10-16.
- Balki M, Chakravarty S, Salman A, et al. Effectiveness of using high-fidelity simulation to teach the management of general anesthesia for cesarean delivery. Can J Anaesth. 2014;61(10):922-934.
- Apfelbaum JL, Hagberg CA, Caplan RA, et al. Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 2013;118(2):251-270.
- Mhyre JM, Healy D. The unanticipated difficult intubation in obstetrics. Anesth Analg. 2011;112(3):648-652.
- Mushambi MC, Kinsella SM, Popat M, et al. Obstetric Anaesthetists’ Association and Difficult Airway Society guidelines for the management of difficult and failed tracheal intubation in obstetrics. Anaesthesia. 2015;70(11):1286-1306.
- Aziz MF, Kim D, Mako J, et al. A retrospective study of the performance of video laryngoscopy in an obstetric unit. Anesth Analg. 2012;115(4):904-906.
- Shonfeld A, Gray K, Lucas N, et al. Video laryngoscopy in obstetric anesthesia. J Obstet Anaesth Crit Care. 2012;2(1):53.
- Browning RM, Rucklidge MW. Tracheal intubation using the Pentax Airway Scope videolaryngoscope following failed direct laryngoscopy in a morbidly obese parturient. Int J Obstet Anesth. 2011;20(2):200-201.
- Kariya N, Kimura K, Iwasaki R, et al. Intraoperative awake tracheal intubation using the Airway Scope in caesarean section. Anaesth Intensive Care. 2013;41(3):390-392.
- Cooper RM. Complications associated with the use of the GlideScope videolaryngoscope. Can J Anaesth. 2007;54(1):54-57.
- Sun DA, Warriner CB, Parsons DG, et al. The GlideScope video laryngoscope: randomized clinical trial in 200 patients. Br J Anaesth. 2005;94(3):381-384.
- Aziz MF, Dillman D, Fu R, et al. Comparative effectiveness of the C-MAC video laryngoscope versus direct laryngoscopy in the setting of the predicted difficult airway. Anesthesiology. 2012;116(3):629-636.
- Van Zundert AA, Kumar CM, Van Zundert TC. Malpositioning of supraglottic airway devices: preventive and corrective strategies. Br J Anaesth. 2016;116(5):579-582.
- Ramachandran SK, Mathis MR, Tremper KK, et al. Predictors and clinical outcomes from failed Laryngeal Mask Airway Unique: a study of 15,795 patients. Anesthesiology. 2012;116(6):1217-1226.
- Timmermann A. Supraglottic airways in difficult airway management: successes, failures, use and misuse. Anaesthesia. 2011;66(suppl 2):45-56.
- Ahuja P, Jain D, Bhardwaj N, et al. Airway changes following labor and delivery in preeclamptic parturients: a prospective case control study. Int J Obstet Anesth. 2018;33(2):17-22.
- Gadd K, Wills K, Harle R, et al. Relationship between severe obesity and depth to the cricothyroid membrane in third-trimester non-labouring parturients: a prospective observational study. Br J Anaesth. 2018;120(5):1033-1039.
- Mhyre JM, Riesner MN, Polley LS, et al. A series of anesthesia-related maternal deaths in Michigan, 1985-2003. Anesthesiology. 2007;106(6):1096-1104.
- Difficult Airway Society Extubation Guidelines Group, et al. Difficult Airway Society Guidelines for the management of tracheal extubation. Anaesthesia. 2012;67(3):318-340.
- Spong AD, Vaughan DJ. Safe extubation of a parturient using an airway exchange technique. Int J Obstet Anesth. 2014;23(3):282-285.
- Chrimes N. The Vortex: a universal ‘high-acuity implementation tool’ for emergency airway management. Br J Anaesth.2016;117(suppl 1):i20-i27.


Leave a Reply
You must be logged in to post a comment.