Abstract
We report profound lip and tongue swelling and hypotension in a 71-year-old woman after anesthesia induction. There was no bronchospasm, urticaria, or rash, so anaphylaxis was not initially suspected. She was treated with phenylephrine, ephedrine and boluses of fluid. When hypotension was refractory to these interventions, she was treated for anaphylaxis with epinephrine, diphenhydramine, and dexamethasone. She had an elevated tryptase level (>7 times), consistent with the diagnosis of anaphylaxis. Subsequent allergy testing was inconclusive. This case report presents an association of isolated lip and tongue swelling with anaphylactic reactions.
Discussion
A perioperative anaphylactic reaction is rare, with a reported incidence of 1 in 6,000 to 1 in 20,000.1 When it happens, anesthesiologists and nurse anesthetists may fail to diagnose the condition due to its variable presentation or coexisting hypotension induced by induction drugs. Multiple etiologies for objective signs of anaphylaxis, such as hemodynamic collapse, high airway pressures, and wheezing, are present in the perioperative milieu. Skin findings may be obscured by surgical drapes, and subjective reports of dyspnea and abdominal symptoms are often impossible to obtain from an anesthetized patient.
Lip and tongue swelling are even rarer presentations of an anaphylactic reaction.2 In 78 severe anaphylactic reactions reported to the Australian Incident Monitoring Study, only 4 cases presented with tongue or airway swelling.2 Here, we present a case report of isolated lip and tongue swelling after anesthesia induction.
Case Report
JD is a 71-year-old woman with a medical history of end-stage renal disease on hemodialysis, type 2 diabetes mellitus, hypertension, hyperlipidemia, coronary artery disease with a drug-eluting stent placed in the left anterior descending artery, and HIV infection. JD presented for deceased donor kidney transplantation.
A preoperative nuclear medicine stress test was negative for inducible ischemia; preoperative lab test results were remarkable only for elevated blood urea nitrogen and creatinine levels; she had no known drug allergies; and her physical exam was otherwise unremarkable. Midazolam was administered prior to transfer to the OR, and induction of anesthesia was achieved with lidocaine, fentanyl, propofol, rocuronium, and sevoflurane.
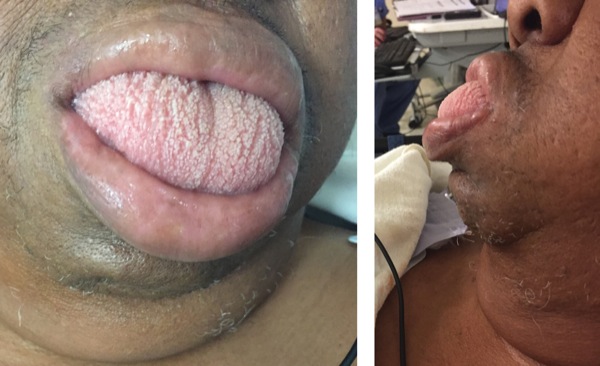
There was immediate concern about tension pneumothorax. Bilateral breath sounds were present without wheezing; ultrasound was used to confirm bilateral sliding signs were present to further exclude pneumothorax. A stat chest x-ray was obtained. Peak airway pressures were normal. The patient’s blood pressure dropped to 45/30 mm Hg and sevoflurane was turned off, but the patient was then noted to have an enlarged tongue, raising concern for anaphylaxis (Figures 1 and 2). The Foley was immediately removed while epinephrine was administered in 3 boluses of 10 mcg each, and dexamethasone and diphenhydramine were administered, which rapidly improved hemodynamics.
Immediately after anesthesia induction, a tryptase level was obtained. It was elevated at 78 mcg/L (reference range, ≤10.9 mcg/L), essentially confirming an anaphylactic reaction. The tryptase value returned to baseline after 24 hours. Further workup was significant for negative latex-specific immunoglobulin E, negative KIT mutation, negative bone marrow biopsy for mast cell disease, and negative test result for hereditary angioedema. Limited drug allergy testing was negative for penicillin, but induction drug testing was not performed.
Conclusion
There are multiple etiologies for isolated tongue swelling, including mechanical trauma, venous/lymphatic outflow obstruction, anaphylaxis, and localized application of chemicals. None but anaphylaxis is associated with hypotension.3
References
- Chacko T, Ledford D. Peri-anesthetic anaphylaxis. Immunol Allergy Clin North Am. 2007;27(2):213-230.
- Currie M, Kerridge RK, Bacon AK, et al. Crisis management during anaesthesia: anaphylaxis and allergy. Qual Saf Health Care. 2005;14(3):e19.
- Grigsby EJ, Lennon RL, Didier EP, et al. Massive tongue swelling after uncomplicated general anaesthesia. Can J Anaesth.1990;37(7):825-826.


Leave a Reply
You must be logged in to post a comment.