Case Presentation
A 28-year-old woman, with morbid obesity (body mass index, 54 kg/m2) with a Mallampati classification II airway presented for placement of a ventriculoperitoneal shunt to address idiopathic intracranial hypertension. After induction of general anesthesia with propofol (2 mg/kg) and succinylcholine (1 mg/kg), endotracheal intubation was attempted with a GlideScope video laryngoscope (Verathon). A 7.0-mm endotracheal tube (ETT) shaped with a GlideRite stylet (Verathon) was inserted into the oral cavity and identified on the video laryngoscope monitor. Although appropriate visualization was achieved on the first attempt, the ETT required several passes prior to entry between the vocal cords, ultimately passing with a 90-degree rightward rotation of the ETT. Appropriate placement was confirmed with bilateral breath sounds, end-tidal carbon dioxide monitoring, and fogging within the ETT.
After completion of the surgery and before extubation, a significant amount of fresh blood was noted when suctioning the oropharynx. Examination of the oropharynx with a Macintosh laryngoscope revealed a right soft palate laceration of 3 cm. The lesion was sutured by an otolaryngologist and good hemostasis was achieved. The patient was extubated uneventfully. At a two-week follow-up visit, the laceration was healed without complications.
Video laryngoscopy (VL) has gained popularity as an efficient tool for management of the elective and difficult airway. A recent Cochrane systematic review of VL versus direct laryngoscopy in adult patients demonstrated a reduced incidence of intubation failure with VL, particularly in difficult airway cases.1 In addition, VL was associated with less upper airway trauma and postoperative hoarseness. However, there are a growing number of publications reporting upper airway trauma using different types of video laryngoscopes.2-9
In a retrospective study, Greer et al reported a higher incidence of soft palate and oropharynx injury with VL (0.234%) compared with direct laryngoscopy (0.015%).7 The authors reviewed the literature, including 20 cases of oropharyngeal trauma. The most common sites of the traumatic injuries were the tonsillar pillars and soft palate, and the most common type of injury was soft tissue through-and-through perforation.7 The tonsillar pillars are particularly susceptible to perforation by the styleted ETT when stretched by excessive force to enable visualization of the laryngeal inlet.8 Most ETTs are inserted with the right hand, so palatal injuries are more frequent on the right side.9 Pham et al reported nine cases of soft palate injury after VL, with six cases involving lacerations to the right palatoglossal arch. Three patients required surgical repair of the soft palate injury, with no complications occurring postoperatively.9
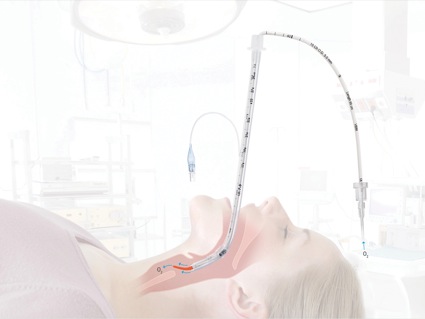
Angulated blade-type video laryngoscopes such as the GlideScope require the use of a curved stylet to advance the ETT into the laryngeal inlet.10 Use of rigid stylets, such as the GlideRite, significantly increase the risk for upper airway injury; therefore, ETTs shaped with malleable stylets can potentially decrease the incidence of traumatic injuries. A standard malleable stylet was reported to be as efficient as a rigid stylet for GlideScope-facilitated endotracheal intubations when used by experienced anesthesiologists.11 The S-guide intubating stylet (VBM Medizintechnik Gmbh) is a new malleable intubating stylet with a soft, preformed, hockey stick–shaped distal tip that may be a valuable alternative to a rigid stylet (Figure).12
Beware the Blind Spot
Watching the video laryngoscope monitor instead of the patient’s mouth when advancing the ETT creates a “blind spot” in the oropharynx where the ETT is not visualized until it is displayed on the camera’s view. To avoid the blind spot, it is recommended to insert the video laryngoscope and the ETT under direct visualization before turning to the monitor screen. Van Zundert recommended switching to the monitor screen view after the ETT is located beyond the uvula.8Using a four-step technique for GlideScope-guided endotracheal intubation is encouraged to avoid traumatic airway manipulation:3,13
- Insert the GlideScope blade midline in the oral cavity under direct visualization.
- Switch to monitor screen visualization to see the epiglottis and glottis opening.
- Insert the ETT in the oral cavity under direct visualization.
- Switch to monitor screen visualization to complete the intubation.
An alternative approach is to place the ETT in the oral cavity before inserting the GlideScope blade.14
When assessing pharyngeal injuries after intubation, other possible causes for oral traumatic injuries should be considered, such as nasogastric or orogastric tube insertion, Yankauer suction tips, and transesophageal echocardiography probes.14
Most of the cases presented in the literature had good outcomes, managed by conservative treatment or surgical suture. Pham et al suggested surgical intervention for through-and-through perforations or large flaps, and administration of prophylactic antibiotics for lesions greater than 1 to 2 cm or those requiring surgical sutures.9
Selected reports of upper airway trauma with different types of video laryngoscopes are listed in the Table. The GlideScope has been in use since 2002 and is one of the most widely used video laryngoscopes. This fact could explain the increased number of reports of oropharyngeal palatal injuries with the GlideScope.
| Table. Reports of Different Sites of Upper Airway Trauma During Video Laryngoscopy | ||
| Type of Injury | Video Laryngoscope | Reference |
|---|---|---|
| Perforation of palatoglossal arch and right tonsil | GlideScope (Verathon) | Nestler C, et al. Anesthesiology. 2013;118(3):709. |
| Laceration of base of tongue | GlideScope (Verathon) | Dupanovic M. J Clin Anesth. 2010;22(2):152-154. |
| Through-and-through perforation of right lateral soft palate | GlideScope (Verathon) | Pagel PS, et al. J Cardiothorac Vasc Anesth. 2019;33(3):873-875. |
| Anterior tonsillar pillar perforation | GlideScope (Verathon) | Malik AM, et al. Anesth Analg. 2007;104(6):1610-1611. |
| Posterior pharyngeal wall laceration | Airtraq (Rusch) | Holst B, et al. Anaesthesia. 2008;63(8):889-890. |
| Right side of soft palate | McGrath (Medtronic) | Williams D, et al. Anaesthesia. 2009;64(10):1141-1145. |
Conclusion
- Most cases of VL-related oropharyngeal lesions had good outcomes, with some necessitating surgical suture and some managed conservatively.
- Gentle manipulation to avoid excessive force is crucial for both direct and indirect techniques for VL.
- Direct visualization of the ETT before it is displayed on the monitor of the video laryngoscope is recommended.
References
- Lewis SR, Butler AR, Parker J, et al. Videolaryngoscopy versus direct laryngoscopy for adult patients requiring tracheal intubation: a Cochrane Systematic Review. Br J Anaesth. 2017;119(3):369-383.
- Pagel PS, Chapel MA, Georgeson AR, et al. An unanticipated airway finding after orotracheal intubation with a GlideScope videolaryngoscope. J Cardiothorac Vasc Anesth. 2019;33(3):873-875.
- Allencherril JP, Joseph L. Soft palate trauma induced during GlideScope intubation. J Clin Anesth. 2016;35:278-280.
- Leong WL, Lim Y, Sia ATH. Palatopharyngeal wall perforation during GlideScope intubation. Anaesth Intensive Care.2008;36(6):870-874.
- Vincent RD Jr, Wimberly MP, Brockwell RC, et al. Soft palate perforation during orotracheal intubation facilitated by the GlideScope videolaryngoscope. J Clin Anesth. 2007;19(8):619-621.
- Hsu WT, Hsu SC, Lee Yl, et al. Penetrating injury of the soft palate during GlideScope intubation. Anesth Analg.2007;104(6):1609-1610.
- Greer D, Marshall KE, Bevans S, et al. Review of videolaryngoscopy pharyngeal wall injuries. Laryngoscope. 2017;127(2):349-353.
- van Zundert A, Pieters B, van Zundert T, et al. Avoiding palatopharyngeal trauma during videolaryngoscopy: do not forget the ‘blind spots.’ Acta Anaesthesiol Scand. 2012;56(4):532-534.
- Pham Q, Lentner M, Hu A. Soft palate injuries during orotracheal intubation with the videolaryngoscope. Ann Otol Rhinol Laryngol. 2017;126(2):132-137.
- Bacon ER, Phelan MP, Doyle DJ. Tips and troubleshooting for use of the GlideScope video laryngoscope for emergency endotracheal intubation. Am J Emerg Med. 2015;33(9):1273-1277.
- Turkstra TP, Harle CC, Armstrong KP, et al. The GlideScope-specific rigid stylet and standard malleable stylet are equally effective for GlideScope use. Can J Anaesth. 2007;54(11):891-896.
- VBM Medizintechnik GmbH. Airway Management. www.vbm-medical.com/ products/ airway-management/ s-guide. Accessed August 10, 2019.
- Pacey JA. In response: anterior tonsillar pillar perforation during GlideScope video laryngoscopy. Anesth Analg. 2007;104:1611.
- Cooper RM. Complications associated with the use of the GlideScope videolaryngoscope. Can J Anaesth. 2007;54:54-57.


Leave a Reply
You must be logged in to post a comment.